Abstract
The healthcare industry aims to enhance life quality and longevity, focusing on equitable access regardless of socioeconomic status, race, or location. Since 1980, the US Department of Health's "Healthy People" initiative has set goals to promote health equity. Private health organizations play a crucial role in addressing Social Determinants of Health (SDoH) to close the equity gap. Even though health equity is a top priority for healthcare executives, it consistently lacks accountability, especially in Puerto Rico, which faces unique challenges such as higher chronic condition prevalence and lower funding.
Private health organizations can drive health equity while also benefiting financially by focusing on three main aspects: 1) Cost Avoidance- Improving health outcomes to reduce higher-cost utilization; 2) Revenue Increase- Enhancing patient loyalty and retention through improved service quality; and 3) Talent Management- Attracting and retaining motivated employees, which enhances organizational performance. To get started, organizations should identify inequities, define strategic goals, evaluate interventions, design effective delivery methods, and monitor progress. Evidence supports that SDoH interventions enhance outcomes and reduce costs, providing a foundation for effective health equity strategies.
Why should my private healthcare organization care about Social Determinants of Health?
More than just treating illnesses, the healthcare industry's mission is to add years to life and life to years. Yet its biggest challenge is ensuring that everyone has equal access to healthcare resources and opportunities regardless of socioeconomic status, race, or location.
Since 1980, the US Department of Health has led the way in promoting health equity with Healthy People, a national initiative to improve the population’s health and well-being. Its focus is high-level and strategic, setting science-based goals and measurable objectives that trickle down and help set priorities in other agencies such as CMS and the CDC. Although the government plays an important role in promoting health equity, other players in the industry, especially private health organizations, could ask themselves why they should care about addressing social determinants of health. And how can they contribute to closing the health equity gap.
Where are we today and what opportunities remain?
According to a recent Bain & Company survey of healthcare executives in the United States, health equity is one of the top five priorities for many organizations (see Figure 1).
Although the same study indicates that they seem to struggle more with applying the same rigor and accountability enforced to other strategic efforts 1, health equity is starting to be prioritized alongside core business strategies.
In Puerto Rico, the extent to which health equity is present in the core business priorities of healthcare executives remains unknown (if you are a healthcare executive working in a private health organization in Puerto Rico, please fill out this 3-minute survey).
After 2019 when CMS changed the criteria for Medicare Part C benefit designs to provide better coverage for Social Determinants of Health (SDoH), Puerto Rico payers have increased their offerings year over year. Most of these are clearly designed to address social determinants of health, such as:
• Transportation to ensure the population has access to doctor appointments or picking up prescriptions, minimizing possible adverse events that lead to ER visits.
• Landscaping services to prevent possible falls or illnesses that arise from poor maintenance of their environment.
• Cash debit cards are eligible to be used for groceries (access to food stability) and essential services like water, electricity, gas, telephone, and internet access.
• Food delivery after hospital stays to ensure food and nutritional security after an acute episode for proper recovery.
• Some plans even provide companionship for MA beneficiaries who request it, giving them someone to talk to, which helps improve their mental health.
Even though these broad benefits are a good starting point, they are exclusively addressing Puerto Rico’s elderly population (~700K lives and a rapidly growing segment.) However, approximately half the island’s population (1.5M) is enrolled in Medicaid 2 (12.5% higher than New Mexico, the next closest state, with 34%.) Our population also has a higher prevalence of chronic conditions as well as less funding and coverage relative to mainland states’ Medicaid programs 3. The Medicare Advantage (MA) benchmark rates on the island remain substantially lower than those in the rest of the country, including other territories. In fact, the 2024 benchmark rate for counties in Puerto Rico is 39% lower than other counties in the U.S. Puerto Rico’s MA 4.
In addition to the valuable benefits provided to MA beneficiaries through Part C, the opportunity exists to direct more attention toward enhancing services for the broader population. However, the going concern of these benefit offerings is put into question for coming years since MA plans are losing money here in Puerto Rico for the first time ever 5.
The bottom line is that private health organizations are uniquely positioned to advance health equity on large scales by addressing social determinants of health within their managed populations while also improving their clinical outcomes and bottom line.
The business case for private health organizations
Integrating Social Determinants of Health into your organization’s strategic priorities and day-to-day operations can improve financial performance in more ways than one:
1) The first and most apparent impact lever is cost avoidance through improved health outcomes.
— Reducing higher cost and/or avoidable utilization such as emergency room visits, hospital admissions, re-admissions and preventable chronic disease development by investing in lower cost preventive care or educational interventions.
2) The second impact lever relates to top line value capture… Increase in revenue through strong patient loyalty.
— Increasing patient attraction and retention through higher net promotor scores (NPS) and overall organizational reputation after implementing an SDoH strategy.
3) The third lever is essential for both top and bottom-line impact… improved talent attraction, retention and performance through sense of purpose.
— Organizations with a motivated and engaged workforce generally perform better than those that don't. Several studies support these claims. For instance, a Gallup study found that companies with highly engaged workforces outperform their peers by 147% in earnings per share and exhibit lower absenteeism, turnover, and safety incidents 6. Similarly, a report by Aon Hewitt indicated that a 5% increase in employee engagement is linked to a 3% increase in revenue growth 7.
All these levers, individually or combined, are likely to yield a positive return-on-investment ROI for your organization. Figure 2 below illustrates a basic ROI formula that considers cost savings and revenue gains from investing in SDOH.
Where:
• Value Capture Gains can include increased revenue from new patients or existing patient retention, better payor contracts or capture of quality metric incentives, as well as reduced costs related to less utilization or reduction of penalties.
• Cost of intervention encompasses the costs of implementing SDoH programs, such as transportation, nutrition assistance, housing, community health workers, etc.
• Increased utilization captures the specific increases in utilization related to the implementation of the SDoH program, such as additional pharmacy or laboratory spend after an educational or access providing SDoH intervention.
It’s important to note that the applicable ROI value capture savings and intervention costs can vary relative to the healthcare organization driving it. For example, increases in non-hospital related patient utilization will likely not be relevant for a hospital provider who is implementing SDoH strategic initiatives. However, as risk-sharing and value-based contracts become a more common way of contracting with payors, it is likely that these become more standardized over time.
Figure 3 below includes some illustrative use cases for different private healthcare organizations where both advancing health equity and improving the bottom line can be achieved.
These use cases are not exhaustive and are meant to serve as simplified practical examples of the most common interventions efforts being documented by the Community Preventive Services Task Force (CPSTF) of the U.S. Department of Health and Human Services (HHS)8. The possible interventions that can be implemented by private organizations to target specific SDOH needs within the managed care population, while meeting its strategic and financial goals are many. The most crucial step is to initiate the process of addressing specific social determinants of health by prioritizing and positioning it in the organization’s overall strategy.
How to get started?
Advancing health equity as a private health organization requires gaining a profound understanding of the disparities impacting patients, establishing appropriate goals with clear and measurable objectives, implementing effective interventions, and having the correct visibility and monitoring mechanisms to measure progress and course correct when needed.
To help your organization get started, we developed a roadmap with 5 clear actionable steps that will guide you in the process of defining, aligning, deploying and monitoring your strategy for SDOH. Figure 4 below illustrates this framework.
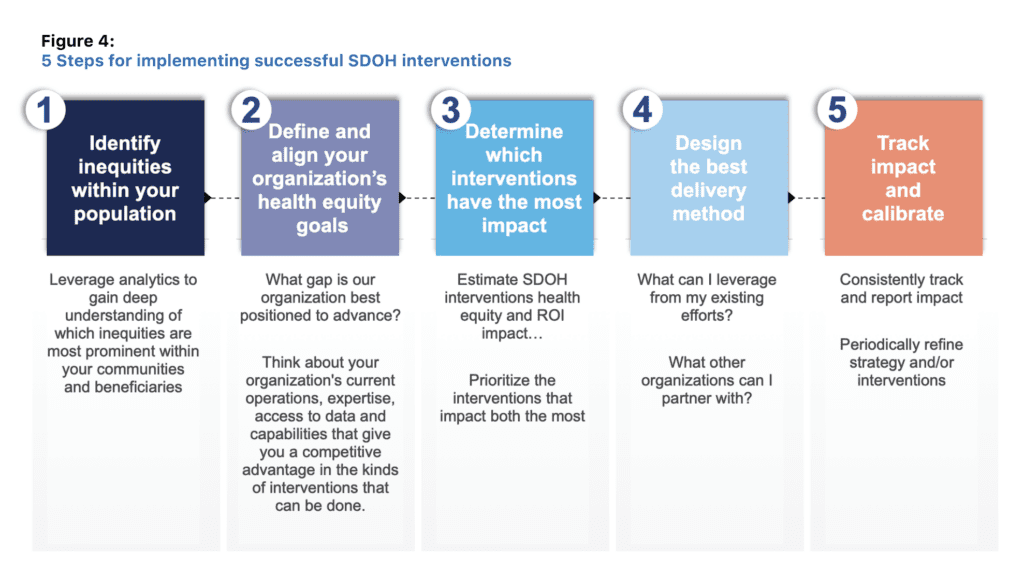
Before defining the organization’s strategic health equity goals, it’s imperative to understand what the biggest health equity gaps are within your population. Defining the organization’s health equity mission without first having a deep understanding of this can lead to interventions that might be aligned with the organization’s strategic and financial goals but have little to no impact on advancing overall health equity. Furthermore, such actions might be perceived as self-serving, undermining the goodwill and loyalty they aim to generate.
To do this it’s important that organizations seek access to racial, environmental, demographic and health data to analyze jointly with their own utilization and/or clinical data to identify where the biggest disparities and opportunities lie.
2. Define and align your organizations strategic health equity goals:
Like any other organization-wide strategy, it is important that health equity goals be defined top-down, where the executive leadership is aligned in allocating funds, time, and resources to support it.
At this stage, the company will determine the mid to long term ambition and goals it will set out to deliver based on answering the question: What health equity gap are we best positioned to improve within our communities/population?
To answer this, you should consider the findings from step 1 and how the organization’s day to day operations, expertise, proprietary data or overall capabilities match their population’s needs and if there is a specific competitive advantage that the organization has over other players in being able to close that inequity gap.
3. Estimate and determine which interventions have the most impact:
In this phase, the business units tasked with determining the interventions required to achieve the previously defined health equity goals, will need to estimate the expected impact. This entails understanding the SDoH being targeted and the potential source of value metrics it impacts with each intervention, creating a baseline with pre-intervention historical data for the targeted population, estimating costs to implement the intervention, and determining the organization’s expected ROI.
These interventions will need to be prioritized based on impact at two levels: 1) closing health equity gaps and 2) impact on the organization’s ROI. Figure 5 below illustrates a useful matrix that can be used to help prioritize interventions.
4. Design and deploy the most effective delivery method:
Each intervention will have very specific operational requirements in terms of resources and capital allocation but not all have to be funded or carried out 100% internally by the organization. In many instances, additional stakeholders, including NGOs or public entities, may already be offering access services or incentives aligned with the eligibility criteria of the population you are focusing on.
At this stage, it is essential to assess potential strategic partnerships with entities exhibiting strong interest and optimal positioning for collaboration, with the aim of engaging them effectively.
5. Monitor results and make adjustments proactively:
Like everything in business, what can’t be tracked can’t be managed. The ability to monitor and assess the impact of the interventions in a timely manner will be key in the successful achievement of the company’s strategic health equity objectives.
Apart from choosing the metrics for monitoring (which will likely be the same ones used to determine impact in step 3), monitoring results will also require:
1. Defining measurable objectives and timeframes based on the chosen metrics.
2. Determining the frequency for gathering, evaluating and reporting each metric (e.g., daily collection for analysis, but monthly assessments with core team members and quarterly reporting to executives).
3. Establishing criteria for expanding, adjusting, or concluding the program.
Conclusion
Year after year, scientific studies show that SDoH interventions can improve health outcomes and well-being as well as decrease health care costs. The HHS is constantly evaluating the effectiveness and impact of SDOH interventions to add them to its evidence-based library6. Although more research is needed to understand what interventions cause the most long-term impact on health outcomes, utilization and costs, the existing literature is useful to get started in defining and implementing your organization’s SDoH goals that will likely have strong short-term impact. Remember to…
1) Start by understanding your population’s most pressing SDoH needs that…
2) …if addressed can help your organization reach its strategic goals.
3) Have clarity on what metrics will drive value capture and estimate your ROI.
4) Partner/coordinate with organizations that share you SDoH goals and are better positioned to deliver the interventions.
5) Measure progress and adjust when needed.
How can we help?
Here at V2A we are passionate about finding ways to improve Puerto Rico’s health outcomes and advance health equity. V2A has and will continue to contribute to this discussion from the perspective of different stakeholders as well as facilitate access to actionable data through our public dashboard of Social Determinants of Health. We encourage you to leverage this tool within your organization’s efforts to better understand where populations most in need can be found. If your organization is interested in collaborating or is looking for support on this topic write to us here.
Sources
1. How to Advance Health Equity While Improving Your Bottom Line | Bain & Company
2. Programa Medicaid - Departamento de Salud
3. Puerto-Rico-2023-Annual-Report-to-Congress_Final-3.pdf (asespr.org)
4. 746c0a_c6b604199d104368b84ecd3b7fa5501e.pdf (mmapapr.org)
5. Con pérdidas millonarias los planes Medicare Advantage en Puerto Rico. - Asociación de Hospitales de Puerto Rico (hospitalespr.org)
6. The Benefits of Employee Engagement (gallup.com)
7. Trends_Global_Employee_Engagement_Final.pdf (aon.com)
8. SDOH-Evidence-Review.pdf (hhs.gov)
Others not directly referenced:
— SDOH Solutions Book - Getting Started with Social Determinants of Health by Derek Wilson
— addressing-the-social-determinants-of-health.pdf (mckinsey.com)
 Coral Frederique Guzmán
Coral Frederique Guzmán




